May 3, 2021
By Dwight Akerman, OD, MBA, FAAO
Just as most primary care optometric practices now routinely utilize threshold visual field and OCT instrumentation, it should be the aim of eye care professionals to do the same for axial length measurement in pediatric myopia management.

Myopia is a refractive condition caused by excessive axial length elongation.1 Once considered a simple refractive error with few, if any, long-term eye health consequences, myopia has now been shown to increase the risk of serious, sight-threatening complications, including myopic macular degeneration, retinal detachment, primary open-angle glaucoma, macular hole, retinoschisis, and nuclear and posterior subcapsular cataract.2
Axial length (AL) measurement has not traditionally been considered part of mainstream optometry. The same could have been said for visual field assessment four decades ago and OCT measurements a decade ago. Just as most primary care optometric practices now routinely utilize threshold visual field and OCT instrumentation, it should be the aim of eye care professionals to do the same for AL measurement in pediatric myopia management.
Recently published work has provided insights into typical AL growth rates, enabling the risk of myopia to be assessed, with normative values being published for a cohort of European and Chinese children.3,4 The collected data were reported as percentiles, a term that is well understood for other growth factors such as height and weight. Children below the 50th percentile for AL increase are significantly less likely to become myopic (and almost certainly not be highly myopic), compared to those above the 50th percentile. Children of Chinese ethnicity have longer axial lengths, indicating the higher prevalence of myopia in that population.
Percentiles of AL in 6-, 9-, and 15-year old European and Chinese children of both genders.3,4
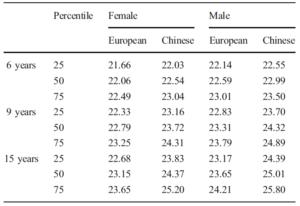
High myopia, which is defined as spherical equivalent (SE) of -6.00D or worse, generally corresponds to AL ≥26 mm, which drastically increases the risk of severe complications later in life. High myopia is currently one of the leading causes of legal blindness in developed countries because of complications occurring in adulthood.5
There are two main options for measuring AL: ultrasound biometry and optical biometry. A-scan ultrasound biometry is not as accurate and a more challenging technique to use on children due to the contact nature of the instrument. There are many options available for optical biometry, covering a range of budget options. Most devices are easy to use on children and are non-invasive.
The main cause of myopia is an increase in axial length. The ocular morbidity increases per millimeter of axial length, and consists of myopic macular degeneration, retinal detachment, primary open-angle glaucoma, macular hole, retinoschisis, and nuclear and posterior subcapsular cataract.2 AL measurement should be considered the gold standard of myopia management.
Here are details of leading optical biometers for measuring axial length:
 Topcon Aladdin-M
Topcon Aladdin-M
Aladdin-M offers an affordable, efficient, and repeatable way to baseline axial length and monitor changes over time. This versatile instrument also includes corneal topography, pupillometry, anterior cornea wavefront analysis, and contact lens fitting tools, making it a comprehensive device for monitoring axial length, evaluating the corneal surface, assessing visual quality, and fitting specialty lenses. Analysis tools plot changes in axial length, refraction, and corneal power; highlight differences in corneal shape between visits; and map higher order aberrations.
The device is easy to use, allowing you to delegate axial length measurements to a technician. Topcon offers a Practice Implementation and Marketing Toolkit to help you integrate this new technology into your practice and promote expanded services to your patients.
 ZEISS IOL Master 700
ZEISS IOL Master 700
The ZEISS IOLMaster 700 utilizes SWEPT Source Biometry with a wavelength of 1,060 nm to measure axial lengths. This approach enables an outstanding measurement repeatability of 8µm of standard deviation of inter-observer repeatability. It also enables the acquisition of a 1mm horizontal B-scan of the macula. This central macula image serves as a fixation check by visualizing the foveal depression. Visibility of the foveal depression indicates fixation of the patient during measurement. The SWEPT Source OCT is also used to derive other axial measurements, such as central corneal thickness, anterior chamber depths, and lens thickness. Keratometry measurements of the ZEISS IOLMaster 700 are derived from an 18-spot 3-zone pattern, repeated 15 times, which allows for effective sampling of corneal irregularities and display of central corneal topography maps. Keratometry measurements are acquired by means of unique telecentric keratometry, which makes the device easy to operate and delegate even to operators not initially familiar with optical biometry.
 NIDEK AL-Scan
NIDEK AL-Scan
The automated AL-Scan optical biometer provides rapid measurements that are essential for clinical efficiency and patient comfort. In 10 seconds, six fundamental values are measured (K, AL, PS, WTW, CCT, ACD). NIDEK’s 3-D auto tracking and auto shot provides the operator with the most ease, comfort, and accuracy on all measurements allowing for enhanced usability.
 Haag-Streit Lenstar Myopia
Haag-Streit Lenstar Myopia
With the Lenstar Myopia, from Haag-Streit, you can accurately measure axial length and track the progression of myopia in young patients based on growth curves provided by myopia experts. Lenstar Myopia consists of the Lenstar 900 optical biometer and the corresponding EyeSuite software, EyeSuite Myopia. The software creates graphics that can help you educate parents on their child’s condition. You can customize and track environmental risk factors such as myopic parents, age of myopia onset, time spent reading or using electronic devices, and time spent outdoors in daylight. EyeSuite Myopia combines all collected data and graphs into a report that provides patients and their parents with information that is easily understandable. This allows them to actively participate in the myopia management process and choose the right treatments relevant to their situation.
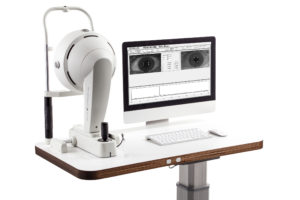 Oculus Pentacam AXL
Oculus Pentacam AXL
The Pentacam AXL is a systematic enhancement of the time-tested Pentacam HR technology. In addition to anterior segment tomography, the original function of its predecessor, the Pentacam AXL has integrated axial length measurement, a feature that allows you to monitor your myopia management patients.
 ARGOS
ARGOS
The ARGOS Optical Biometer with Image Guidance by Alcon is a non-invasive, non-contact optical biometer that uses SS-OCT (swept-source optical coherence tomography) to capture six OCT images of the eye in less than one second and outputs three sets of results with calculated average and standard deviation values for nine parameters: axial length, corneal thickness, anterior chamber depth, lens thickness, pupil size, corneal diameter, flat meridian, steep meridian, and astigmatism. In addition, a reference image is taken at the same time. Unique to ARGOS, a real-time whole eye 2D OCT image is displayed during measurement. Correct alignment can be quickly established, assuring confidence for a measure well taken. The post measurement analyze screen shows the whole eye image with boundary markers, which ensures measurement plausibility and a visual segmentation/
References
1 Meng, W., Butterworth, J., Malecaze, F., & Calvas, P. (2011). Axial length of myopia: a review of current research. Ophthalmologica, 225(3), 127-134.
2 Haarman, A. E., Enthoven, C. A., Tideman, J. W. L., Tedja, M. S., Verhoeven, V. J., & Klaver, C. C. (2020). The Complications of Myopia: A Review and Meta-Analysis. Investigative Ophthalmology & Visual Science, 61(4), 49-49.
3 Tideman, J. W. L., Polling, J. R., Vingerling, J. R., Jaddoe, V. W., Williams, C., Guggenheim, J. A., & Klaver, C. C. (2018). Axial length growth and the risk of developing myopia in European children. Acta ophthalmologica, 96(3), 301-309.
4 Diez, P. S., Yang, L. H., Lu, M. X., Wahl, S., & Ohlendorf, A. (2019). Growth curves of myopia-related parameters to clinically monitor the refractive development in Chinese schoolchildren. Graefe’s Archive for Clinical and Experimental Ophthalmology, 257(5), 1045-1053.
5 Tideman, J. W. L., Snabel, M. C., Tedja, M. S., Van Rijn, G. A., Wong, K. T., Kuijpers, R. W., … & Boon, C. J. (2016). Association of axial length with risk of uncorrectable visual impairment for Europeans with myopia. JAMA ophthalmology, 134(12), 1355-1363.













