sponsored content
September 15, 2022
By Andrew Biondo, OD
In our office, using the fit sets has become second nature. We’ve developed and perfected a system that works for everyone in the office, and it has changed the way we’re able to prescribe OrthoK lenses.
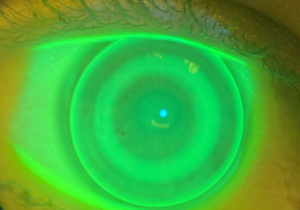
Using an OrthoK fit set helps Dr. Biondo assess how the lens sits on patients’ eyes.
I’ve fitted patients with orthokeratology lenses for the last decade. It was a treatment option I had initially just dipped my toe into but grew more comfortable with and could prescribe for more patients. Seeing patients and parents get excited about the outcomes, and being able to share other patient success stories, has made all the difference in my practice.
When I started prescribing OrthoK, I used a fitting set with my patients. I was gifted a fitting set from a retiring doctor, and that’s how I initially got into it. Over time, I moved into empirical fits, and while I had success with them, I eventually made my way back to the fitting sets. Even though OrthoK has been FDA approved for the temporary reduction of myopia for 20 years, for many of the parents we talk to, it’s still a relatively new idea and can be a bit unnerving. It’s important to me to have a higher level of success with my patients right out of the gate, and if a patient isn’t responding to the treatment appropriately, skepticism starts to kick in quickly.
Empirical Fits vs. Fit Sets
Several factors come into play when thinking about fitting empirically or using a fitting set. I always have to consider the measurements I’m taking and what that will translate to when the lens is on the patient’s eye. There are a dozen ways to get the measurements we need to design a lens. You’ll get a perfect lens if you have perfect measurements and the math works out. But it can be challenging to get perfect measurements on kids. They don’t always sit still, and you don’t always get the most accurate refractions. When I put a lens on a child’s eye in the exam room, I know I will be able to identify the correct treatment zone and eliminate any errors.

OrthoK fitting sets help manage patients’ expectations of the lenses and measure their comfort levels.
We also have to consider that many of our patients have never had a lens like this on their eyes before. When we order an empirical fit and put it on the patient, they’re sometimes unhappy with the comfort. These aren’t always highly comfortable initially, or they may be the wrong fit, which could deter the patient from moving forward. That’s why it helps to have the lens on the eye and give them a feel for it.
When using the fit set, I can put the trial lens on the patient’s eye for 20 to 30 minutes and see how they do with it. They close their eyes, and I can observe where the lens is sitting in a closed-eye state, even though it’s not necessarily overnight. This is beneficial for a few reasons. For starters, it helps the patient get comfortable immediately with what this lens will feel like when they go to sleep. With empirical designs, you send the patient home with the lens, and you don’t know how the lens is sitting on the eye, and you won’t until the next day. That troubleshooting aspect is what we try to do with the fitting sets. This also gives us instant feedback on how the lens may help the patient long-term. When they have the lens on for 20 to 30 minutes, and we check their acuity immediately, low myopes are seeing 20/20 for a few minutes — even after just a short stint in the lenses. This demonstration helps build patient confidence and helps parents feel more comfortable that this treatment will do what it’s designed to do.
Improving Chair Time
Using both a fitting set and fitting patients empirically, I’ve learned that fit sets are a big saver for chair time and follow-up visits in my practice. It’s easier to take 10 or 20 minutes up-front at the dispensing and get it right, as opposed to having the patient come back and take up another spot on your schedule. It’s also important to me to get the lenses right the first time for my patients – that goes a long way with patients and their parents.
The number of visits is critical for me. Anything we can do to reduce the number of visits increases profitability, success, and patient confidence. Getting the right fit the first time without any guesswork is extremely valuable for my time – because chair time is a monetary system – and my patients and their parents’ time. One of the metrics we use in our practice is revenue per exam, so we know what we’re supposed to get monetarily from each chair-time visit. If we have to give an extra one of those up, that’s revenue we’re losing by not doing it right the first time. The more time we give up as ECPs, the less return we get – especially across our entire patient base. For my patients and their families, their time is just as valuable. Kids have activities, school, and siblings. The fewer times they need to return to the office, the better. It may take a few extra minutes on the front end to use the fit set, but it reduces the number of visits on the back end, which benefits our patients and our practice.
In our office, using the fit sets has become second nature. We’ve developed and perfected a system that works for everyone in the office, and it has changed the way we’re able to prescribe OrthoK lenses. There are always factors during overnight wear that we can’t account for, but we can at least do everything possible on the front end to mitigate as many of those concerns as possible.
This article is sponsored by X-Cel Specialty Contacts.
 |
Dr. Andrew Biondo owns Kirkwood Eye Associates in St. Louis, a specialty contact lens practice with the objective of delivering an exceptional experience for patients and the community. They also have a large myopia control practice that utilizes orthokeratology, atropine, and other specialty contact lenses. Dr. Biondo serves as a consultant to the specialty contact lens industry and speaks internationally on specialty contact lenses and practice management. He is a fellow of the Scleral Lens Education Society and a past president of the St. Louis Optometric Society. |













