April 1, 2020
By Xiangui He, MD, PhD
 Myopia, characterized by onset and rapid progression in childhood, is already a global health threat in East and Southeast Asia, with nearly half of school students aged 12 years and older myopic.1, 2 Myopia can be corrected with spectacles, contact lenses, or refractive surgery, and its progression often slows down in late childhood or early adulthood. However, the increasing trend of myopia manifesting at an earlier age is increasing the risk of an individual reaching high myopia.3 Some regions in Asia are already witnessing an epidemic of high myopia in children and young adults.2, 4, 5 Several ocular complications occur in patients with high myopia at older ages. One such complication, myopic maculopathy, is now the leading cause of irreversible and usually bilateral visual impairment among working populations in East Asia.6-8 Therefore the presence of high myopia will inevitably lead to the substantial reduction of life quality in both children and adults, and it will considerably increase the economic burden in managing them.9, 10
Myopia, characterized by onset and rapid progression in childhood, is already a global health threat in East and Southeast Asia, with nearly half of school students aged 12 years and older myopic.1, 2 Myopia can be corrected with spectacles, contact lenses, or refractive surgery, and its progression often slows down in late childhood or early adulthood. However, the increasing trend of myopia manifesting at an earlier age is increasing the risk of an individual reaching high myopia.3 Some regions in Asia are already witnessing an epidemic of high myopia in children and young adults.2, 4, 5 Several ocular complications occur in patients with high myopia at older ages. One such complication, myopic maculopathy, is now the leading cause of irreversible and usually bilateral visual impairment among working populations in East Asia.6-8 Therefore the presence of high myopia will inevitably lead to the substantial reduction of life quality in both children and adults, and it will considerably increase the economic burden in managing them.9, 10
Although the exact mechanism underlying the onset of myopia is unclear, research indicates an interaction between genetic and environmental factors.11 A higher correlation in refractive error between monozygotic twins than dizygotic twins and a higher risk of children with parental myopia developing into myopia was observed, indicating the role hereditary factors play in the development of myopia.12, 13 But whether these family correlations are the reflection of shared environment or shared genes needs further verification. Mutations or variations of numerous genetic loci have been demonstrated to be associated with early-onset or familial high myopia. However, determinant genes that could be applied practically as intervention methods to delay its onset have not been discovered yet.14, 15 On the other hand, evidence of the critical, influential effect of environmental factors is increasing with decreased outdoor activity and increased educational burden as some of the likely factors underlying the rising trajectory of school myopia.11, 20
What is effective in preventing or delaying the onset of myopia in school children?
Several studies have indicated that improving outdoor time is effective in delaying or preventing the onset of myopia in school children.16-20 An outdoor exposure of approximately 10 to 14 hours per week seems to be able to reduce the risk of onset despite high amounts of near work or parental myopia.21 School-based randomized trials have also demonstrated that encouraging children to go outside for activities during recess or simply adding one additional 40-minute class of outdoor activities were effective in reducing incident myopia .16-18 And it appears that factors related to light rather than physical activity or sport might be an important factor driving the protective effect of outdoor time.21, 22 Other strategies that are currently trialed include the use of low dose atropine (ATOM 3 study) with the clinical trial still in progress.
How to implement time outdoors – how much, what time of day or location, and should it be continuous?
The first issue is the amount of time outdoors. In this regard, a meta-analysis suggests that there is an inverse relation with increased time outdoors associated with a lowered risk of incident myopia. 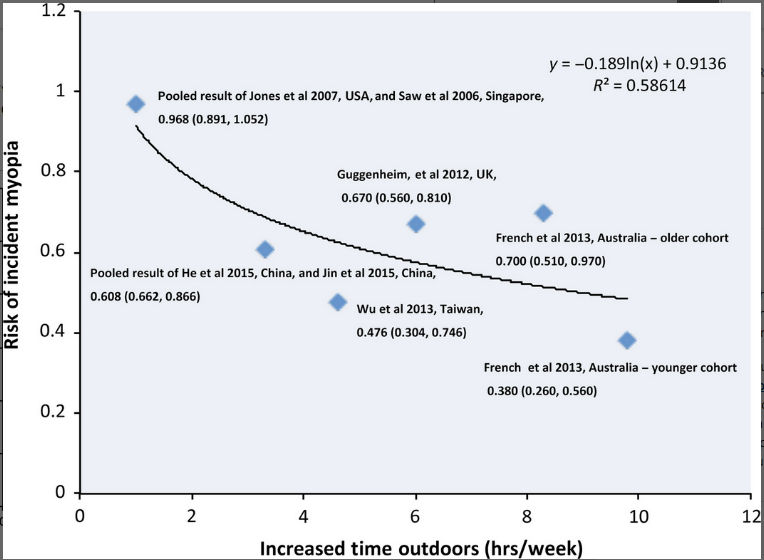 An increase of about 76 minutes per day from baseline time reduced the risk of incident myopia by 50 percent, whereas 60 minutes per day reduced the risk by 45 percent.20 Results of an ongoing randomized trial investigating the effect of outdoor time using objective methods have also observed similar dose-response effect (data not published).19 The second issue is the timing, i.e., continuous or discontinuous, morning or noon. In this regard, the evidence is not clear, and further research is needed. Still, the limited information studies seem to suggest that discontinuous outdoor time (going outside during every recess) may be as useful as continuous (one additional 40-minute class of outdoor activities).16, 17 Since light intensity differs during different periods of the day, the protective effect of outdoor time might also vary during the day. Still, there have been no data so far on whether there is an optimum time of the day that promotes the protective effect. The third issue relates to the location. For example, is it sufficient if the child is in a hallway or corridor in indirect light, or should it be direct light? Both the intensity and duration of light exposure affect the protective effect of outdoor time, and their interactive relation could help identify the optimal locations. Results of a study by Wu et al. implied that outdoor activities with relatively lower outdoor light intensity (such as in hallways or under trees) might help but require a longer time outdoors to be effective.18
An increase of about 76 minutes per day from baseline time reduced the risk of incident myopia by 50 percent, whereas 60 minutes per day reduced the risk by 45 percent.20 Results of an ongoing randomized trial investigating the effect of outdoor time using objective methods have also observed similar dose-response effect (data not published).19 The second issue is the timing, i.e., continuous or discontinuous, morning or noon. In this regard, the evidence is not clear, and further research is needed. Still, the limited information studies seem to suggest that discontinuous outdoor time (going outside during every recess) may be as useful as continuous (one additional 40-minute class of outdoor activities).16, 17 Since light intensity differs during different periods of the day, the protective effect of outdoor time might also vary during the day. Still, there have been no data so far on whether there is an optimum time of the day that promotes the protective effect. The third issue relates to the location. For example, is it sufficient if the child is in a hallway or corridor in indirect light, or should it be direct light? Both the intensity and duration of light exposure affect the protective effect of outdoor time, and their interactive relation could help identify the optimal locations. Results of a study by Wu et al. implied that outdoor activities with relatively lower outdoor light intensity (such as in hallways or under trees) might help but require a longer time outdoors to be effective.18
How to reach out to a child who is not yet myopic
Improved outdoor time is a preventative strategy to reduce future risk of myopia, and such preventative strategies typically require many stakeholders, i.e., public, practitioners, community groups, public health organizations, policymakers, and other relevant groups to work together to educate and intervene appropriately. Strategies to improve the uptake may vary depending on who is involved. For example, if a practitioner is engaged, they may want to consider discussing with parents/care providers of young children the importance of promoting and providing a favorable outdoor environment. Or they may adopt local schools in their area and be actively involved in promoting the eye health of young children in their community by screening young children and educating their community. On the other hand, public health organizations may work with policymakers to educate the public to raise their awareness or work with schools and other relevant bodies to drive more parents to have their children’s vision assessed and improve time outdoors.
An initial screening is necessary to assess the refractive status of children, to identify those at higher risk of developing myopia. Children may be classified based on age, refractive status, and risk factors and recommendations or interventions provided accordingly. Normal developmental refractive stage refers to hyperopia with spherical equivalent > +1.00D in kindergarten children (age 5-6), +0.75D in primary school children (6-12 years), and +0.50D in secondary school children (>12 yrs).1 In addition to advising on outdoor time, children at higher risk of myopia may need an evaluation of other risk factors (for example, near work), and any treatment plan including customized follow-up based on the assessment.
In summary, ongoing research utilizing objective measurements and varying doses may shed further light on mechanisms underlying the protective effect and provide more specific methods for improved efficacy. Still, it is clear from the available data that presently improved outdoor time is the only effective, evidence-based tool known to slow onset of myopia.

Xiangui He, MD, PhD, is Associate Chief Physician of Public Health, Director of Clinical Research Center, Executive Director of Children Myopia, Department of Preventative Ophthalmology, Shanghai Eye Disease Prevention & Treatment Center, Shanghai Eye Hospital, Shanghai, China
References
- Ma Y, Qu X, Zhu X, et al. Age-Specific Prevalence of Visual Impairment and Refractive Error in Children Aged 3-10 Years in Shanghai, China. Invest Ophthalmol Vis Sci 2016;57(14):6188-96.
- Yotsukura E, Torii H, Inokuchi M, et al. Current Prevalence of Myopia and Association of Myopia With Environmental Factors Among Schoolchildren in Japan. JAMA Ophthalmol 2019.
- Holden BA, Fricke TR, Wilson DA, et al. Global Prevalence of Myopia and High Myopia and Temporal Trends from 2000 through 2050. Ophthalmology 2016;123(5):1036-42.
- Wang SK, Guo Y, Liao C, et al. Incidence of and Factors Associated With Myopia and High Myopia in Chinese Children, Based on Refraction Without Cycloplegia. JAMA Ophthalmol 2018;136(9):1017-24.
- Guo Y, Duan JL, Liu LJ, et al. High myopia in Greater Beijing School Children in 2016. PLoS One 2017;12(11):e0187396.
- Chen Q, He J, Hu G, et al. Morphological Characteristics and Risk Factors of Myopic Maculopathy in an Older High Myopia Population-Based on the New Classification System (ATN). Am J Ophthalmol 2019;208:356-66.
- Wu JF, Bi HS, Wang SM, et al. Refractive error, visual acuity and causes of vision loss in children in Shandong, China. The Shandong Children Eye Study. PLoS One 2013;8(12):e82763.
- Xu L, Wang Y, Li Y, et al. Causes of blindness and visual impairment in urban and rural areas in Beijing: the Beijing Eye Study. Ophthalmology 2006;113(7):1134.e1-11.
- Jones D, Luensmann D. The prevalence and impact of high myopia. Eye Contact Lens 2012;38(3):188-96.
- Naidoo KS, Fricke TR, Frick KD, et al. Potential Lost Productivity Resulting from the Global Burden of Myopia: Systematic Review, Meta-analysis, and Modeling. Ophthalmology 2019;126(3):338-46.
- Morgan IG, French AN, Ashby RS, et al. The epidemics of myopia: Aetiology and prevention. Prog Retin Eye Res 2018;62:134-49.
- Hammond CJ, Snieder H, Gilbert CE, Spector TD. Genes and environment in refractive error: the twin eye study. Invest Ophthalmol Vis Sci 2001;42(6):1232-6.
- Liao C, Ding X, Han X, et al. Role of Parental Refractive Status in Myopia Progression: 12-Year Annual Observation From the Guangzhou Twin Eye Study. Invest Ophthalmol Vis Sci 2019;60(10):3499-506.
- Jin ZB, Wu J, Huang XF, et al. Trio-based exome sequencing arrests de novo mutations in early-onset high myopia. Proc Natl Acad Sci U S A 2017;114(16):4219-24.
- Cai XB, Shen SR, Chen DF, et al. An overview of myopia genetics. Exp Eye Res 2019;188:107778.
- Wu PC, Tsai CL, Wu HL, et al. Outdoor activity during class recess reduces myopia onset and progression in school children. Ophthalmology 2013;120(5):1080-5.
- He M, Xiang F, Zeng Y, et al. Effect of Time Spent Outdoors at School on the Development of Myopia Among Children in China: A Randomized Clinical Trial. Jama 2015;314(11):1142-8.
- Wu PC, Chen CT, Lin KK, et al. Myopia Prevention and Outdoor Light Intensity in a School-Based Cluster Randomized Trial. Ophthalmology 2018.
- He X, Sankaridurg P, Xiong S, et al. Shanghai Time Outside to Reduce Myopia trial: design and baseline data. Clin Exp Ophthalmol 2019;47(2):171-8.
- Xiong S, Sankaridurg P, Naduvilath T, et al. Time spent in outdoor activities in relation to myopia prevention and control: a meta-analysis and systematic review. Acta Ophthalmol 2017.
- Rose KA, Morgan IG, Ip J, et al. Outdoor activity reduces the prevalence of myopia in children. Ophthalmology 2008;115(8):1279-85.
- Read SA, Collins MJ, Vincent SJ. Light exposure and eye growth in childhood. Investigative Ophthalmology and Visual Science 2015;56(11):6779-87.
- He X, Zhao R, Sankaridurg P, et al. Design and methodology of the Shanghai child and adolescent large-scale eye study (SCALE). Clin Exp Ophthalmol 2018;46(4):329-38.
Figure 1. Dose-response analysis indicating an inverse relation between time outdoors and the risk of incident myopia (y: risk ratio; and x: increased time spent outdoors) (cited from Xiong et al. Acta Ophthalmol 2017, 95(6):551-566).













