April 12, 2019
By Daniel Press OD, FCOVD
Review of Optometric Business, December 2018
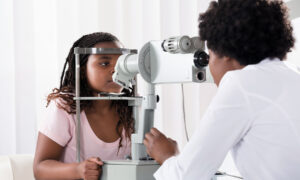
For most eyecare professionals (ECPs), progressive myopia, especially among children, is a refractive error that they correct with single vision spectacles or contact lenses. We must stop thinking about myopia as simply a refractive error and start thinking about it as an eye health issue. Progressive myopia should be a concern for all ECPs, as it is associated with an increased risk of blinding eye diseases such as cataracts, glaucoma, retinal detachment, and myopic macular degeneration.1
Technology is an important consideration in myopia management. What technology assists in developing baseline measurements of myopia? What technology is beneficial for monitoring myopia progression? What technology is being used in the treatment of progressive myopia? Before answering these questions, defining myopia as more than subjective distance blur is helpful. Myopia leads to blurred distance vision, but the true concern is related to the increased axial length of the eye. Defining myopia in relation to axial length will help communicate that true concern to patients.
Why is it that the rates of myopia are skyrocketing worldwide? Due to the rapid increase in the prevalence of myopia from this generation to the last, it is believed that environmental factors are playing a significant role in the alarming rates of myopia. The advent and infiltration of technology over the previous two decades is thought to be partially responsible for the myopia surge.
There are active debates as to the role of near point stress and increasing myopia, but what has been shown repeatedly is that sunlight exposure is correlated with lower levels of myopia. Could it be simply that children are spending more time on technology and less time playing outside?
Technology and causation: screen time
Technology and screen time should be a concern for parents and ECPs alike. When advising patients, the American Academy of Pediatrics has resources available for parents on the subject.2 Sunlight/daylight has been shown to reduce the risk of developing myopia and in addition has been shown to possibly reduce the progression of myopia.3,4,5 Currently parental report is the only way to assess time outdoors.

Technology to monitor light exposure in children would be useful data for the ECP, but what could be used to accomplish that purpose? Wearable technology that does not promote increased screen time, such as the GizmoWatch is gaining popularity among parents with younger children. The GizmoWatch is a kid-friendly smartwatch that does not encourage “screen addiction.”6 It is being marketed as a way to keep children safe. The watch allows for limited access to messaging and phone calls and has a GPS locator. It would be feasible to add sunlight monitoring to the existing technology which would give important information to parents and practitioners.
The educational environment is emphasizing more use of digitaltechnology in and outside of the classroom. It is estimated that half of students in the United States have school-issued technology. There are a reported 30 million children in the U.S. that use Google’s education apps. Combine that with recreational, social and gaming use of technology, and the outlook is grim for how much time children are spending on screens.
Tech companies are beginning to recognize the concern, and new software is allowing parents to monitor screen time. For example, Apple iPhone’s operating software version ios-12 has screen time insight capabilities. Not only can you monitor screen time, but you can adjust the settings to control downtime. ECPs should be equipped to educate parents on the concerns related to screen time and encourage limiting recreational screen time in the household.
Genetics & environment
Currently, we understand the risk factors for myopia to include genetic and environmental components. The number of myopic parents is a risk factor for a child developing myopia. Is that directly due to genetic risk or is that due to cultural influences? The most likely answer is that it is due to a combination. Much work has been done in the area of genetics and myopia, and recent research has identified 161 genetic factors in myopia.7 In the future, understanding how a different genetic makeup interacts with different environmental influences will aid in establishing a comprehensive myopia baseline. This potentially allows the ECP to identify at-risk patients, make specific environmental recommendations and tailor treatments to target the patient who may respond better to specific optical or pharmaceutical intervention.
Develop a baseline and monitor
Once a child shows risk factors or is developing myopia, technology can play an important role in developing a baseline and monitoring progression. Currently, there is ample evidence supporting three methods for slowing myopia progression. Two interventions (orthokeratology and multifocal contact lenses) involve optical defocus, and one intervention (atropine ophthalmic solution) involves a biochemical influence. The technologies incorporated in practice should allow for the measurements of visual/ocular components that may contribute to the development of myopia or are potentially influenced by the interventions. Those components include axial length, cornea, pupil size, accommodation, and binocular vision.
Increased axial length is a risk factor for permanent visual loss.8 An important question that is yet to be answered is what is considered satisfactory control in regards to axial length? While we wait for the data from randomized clinical trials, axial length information is critical in determining the effectiveness of any myopia intervention program, and it will likely be considered standard of care for myopia management in the near future. Axial length is measured by either ultrasound biometry or non-contact optical biometry.
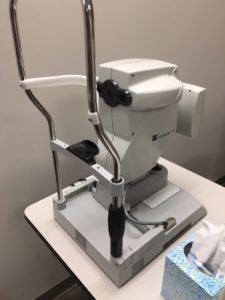
The IOL Master from Zeiss provides valuable axial length data, which is useful in guiding decision making in myopia management.
Contact ultrasound biometry is not utilized often in clinical practice due to the difficulty in conducting the examination, particularly in the pediatric population. Therefore, the most common technology employed in measuring axial length is optical biometry. Among the available optical biometry options, the most common technology used in research and clinical practice is the IOLMaster from Zeiss and the Haag-Streit Lenstar. The ECP can expect to spend in the range of $12,000-$15,000 for a refurbished IOLMaster 500 from Zeiss. In addition to providing valuable information, investing in this technology will help establish the clinic as one that is serious about actively managing myopia.
Corneal analysis, contact lens fitting & topography
Corneal analysis is critical for contact lens fitting, especially if fitting orthokeratology lenses. There are new technologies that combine biometry and topography. Examples of these technologies include the Aladdin HW3.0 by Topcon and the Pentacam AXL by Oculus. The prices for these technologies are likely not justified for the primary care optometrist looking to get started in the field of myopia management.
Placido-based topographers would likely be the most reasonable choice, and is considered standard of care when fitting orthokeratology lenses. Options include the Keratograph 5m by Oculus and the E300 by Medmont. The Keratograph 5m excels not only in the measurement of corneal topography but has the advantage of dry eye diagnostics and pupillometry. The E300 has the advantage with taking precise measurements with impressive accuracy and the broadest coverage of the placido disk topographers. Other technology that is helpful but not considered standard of care is wavefront aberrometry, useful in understanding higher order aberrations in the optical system.

The Keratograph by Oculus is one of the many options for topographic measurement of the cornea. Topography is essential for monitoring patients undergoing orthokeratology treatment, and it provides valuable information for many conditions affecting the cornea.
Pupil size is critical information for the ECP when managing myopia. Objective pupillometry provides information that can be used to design optics that target the peripheral retina. In addition, pupillometry can aid in quantifying the mydriatic side effect of atropine ophthalmic solution, an increasingly common tool in combating progressive myopia. Objective pupil size can be measured with independent technology such as the VIP-300 by Neuroptics, which has the benefits of measuring pupil size under different lighting conditions. Alternatively, most topographers will allow for the basic objective measurements of pupil size.
Technology & treatment: peripheral myopic defocus
The effectiveness of therapies for myopia utilizing optical defocus are dependent on the leading theory of peripheral myopic defocus slowing myopia progression. Technologies relying on peripheral defocus include overnight orthokeratology, daytime wear multifocal contact lenses and, more recently, spectacle designs incorporating defocus technology.
A new spectacle lens, the MyoSmart lens by Hoya, developed in cooperation with the Hong Kong Polytechnic University, has multiple small spheres of defocus immediately outside of a clear central optic zone. A single study that was a two-year, randomized, double-blind trial showed impressive results at slowing axial elongation. Although the early evidence for the MyoSmart Lens is compelling, the eyecare practitioner should keep in mind it currently is available only in Asia.MyoSmart spectacle lenses are due for a global launch in the next two years. Another spectacle lens explicitly designed to slow the progression of myopia is the Zeiss MyoVision Pro. More study is needed in the utility of this new lens in slowing myopia progression.
Single-use (daily disposable) soft contact lenses are an attractive option for pediatric patients due to their superior safety profile. Single-use contact lenses that have promising roles in myopia management through peripheral defocus include the NaturalVue 1 Day Multifocal by VTI and the MiSight daily lenses by CooperVision (currently not available in the U.S.). Currently, there is no product design or medication that is FDA-approved for specifically reducing the progression of myopia.
Beyond those two designs, extended depth of focus contact lenses recently have been developed by the Brien Holden Vision Institute based in Australia.
Orthokeratology
Orthokeratology (OK) has been indicated for the temporary reduction of myopia but also has been shown to reduce the progression of myopia.9 The research supporting the use of OK lenses in reducing myopia progression have most often used designs of contact lens manufacturers Paragon and Euclid, which have a standard optic zone size. Designing OK lenses that control the amount of plus power in the periphery by controlling the size of the optic zone may prove to be even more effective at slowing myopia progression than what has been shown to date. OK technology that allows for better outcomes for patients with astigmatism is also available through Paragon, Euclid, and EyeSpace, among others.
Atropine
Atropine ophthalmic solution is currently the only pharmaceutical option available in the U.S. that has been shown to slow myopia progression. The most common use of atropine is with lower concentrations, as low as 0.01 percent. While on therapy it is known that the higher the concentration of atropine, the more effective the treatment.10,11 Side effect profiles should be monitored in patients on atropine therapy, and that includes measuring accommodation and pupil size. Due to the side effects of atropine, other molecules are being explored for effectiveness of myopia control while minimizing side effects.
While atropine is a non-selective muscarinic antagonist, Pirenzepine is a selective muscarinic antagonist that does not cause mydriasis and cycloplegia. While Pirenzepine has shown positive results in slowing myopia progression, clinical trials in the U.S. have been discontinued due to intolerance by subjects. Other future possibilities in pharmaceutical intervention include the use of Dopamine, Nitric Oxide, Growth Factors, Gamma-aminobutyric Acid, and 7-methylzanthine (7-MX).12 7-MX is of particular interest as it is a metabolite of caffeine and dark chocolate making for good headlines!
This is an exciting time in the field of myopia management. We are still in the nascent phase of understanding how environmental, genetic, optical, pharmaceutical and other factors influence the development and progression of myopia. Existing and emerging technologies in contact and spectacle lenses, pharmaceuticals and diagnostic equipment are enhancing our ability to identify and treat patients suffering from progressive myopia. While there is a plethora of information available on the topic of myopia, the ECP interested in providing this critically important service in the clinical setting will have a tremendous amount of new information to look forward to in these next few years.
- Flitcroft, D. I. (2012). The complex interactions of retinal, optical and environmental factors in myopia aetiology. Progress in retinal and eye research, 31(6), 622-660.
- https://www.aap.org/en-us/about-the-aap/aap-press-room/Pages/American-Academy-of-Pediatrics-Announces-New-Recommendations-for-Childrens-Media-Use.aspx
- Effect of outdoor activity on myopia onset and progression in school-aged children in northeast China: the Sujiatun Eye Care Study, Ju-Xiang J et al. BMC Ophthalmology 2015 15:73
- Risk factors for incident myopia in Australian schoolchildren: the Sydney adolescent vascular and eye study. French AN, et al. Ophthalmology. 2013 Oct;120(10):2100-8
- Myopia Prevention and Outdoor Light Intensity in a School-Based Cluster Randomized Trial. Wu PC, Chen CT et al. Ophthalmology. 2018 Aug;125(8):1239-1250. doi: 10.1016/j.ophtha.2017.12.011. Epub 2018 Jan 19.
- https://www.verizonwireless.com/connected-devices/verizon-gizmowatch/
- Genome-wide association meta-analysis highlights light-induced signaling as a driver for refractive error, Nature Genetics (2018)
- Association of Axial Length With Risk of Uncorrectable Visual Impairment for Europeans With Myopia. Tideman, Snabel, et al. JAMA Ophthalmol. 2016 Dec 1;134(12):1355-1363
- Orthokeratology for Myopia Control: A Meta-analysis. Jun-Kang, et al. Optometry & Vision Science: March 2015 – Volume 92 – Issue 3 – p 252–257
- A Review of Current Concepts of the Etiology and Treatment of Myopia. Cooper J, Tkatchenko AV Eye and Contact Lens Vol 44;4;2018
- Yam, Jiang, et al. Low-Concentration Atropine for Myopia Progression (LAMP) Study: A Randomized, Double-Blinded, Placebo-Controlled Trial of 0.05%, 0.025%, and 0.01% Atropine Eye Drops in Myopia Control. Ophthalmology. 2018
- The Science Behind Myopia. 2017 Nov 7. Carr BJ, Stell WK. In: Kolb H, Fernandez E, Nelson R, editors. Webvision: The Organization of the Retina and Visual System [Internet].
Daniel Press, OD, FCOVD is in private practice at North Suburban Vision Consultants, located in the north suburbs of Chicago, where he serves as the director of pediatrics, binocular vision and vision therapy. Dr. Press is board certified by the College of Optometrists in Vision Development (COVD) in vision therapy and rehabilitation and currently serves on the COVD board of directors as President-Elect. Dr. Press has authored articles and is a frequent lecturer on the topics of myopia and visual development and rehabilitation. Dr. Press is adjunct faculty at ICO, IU School of Optometry, SUNY and PCO.